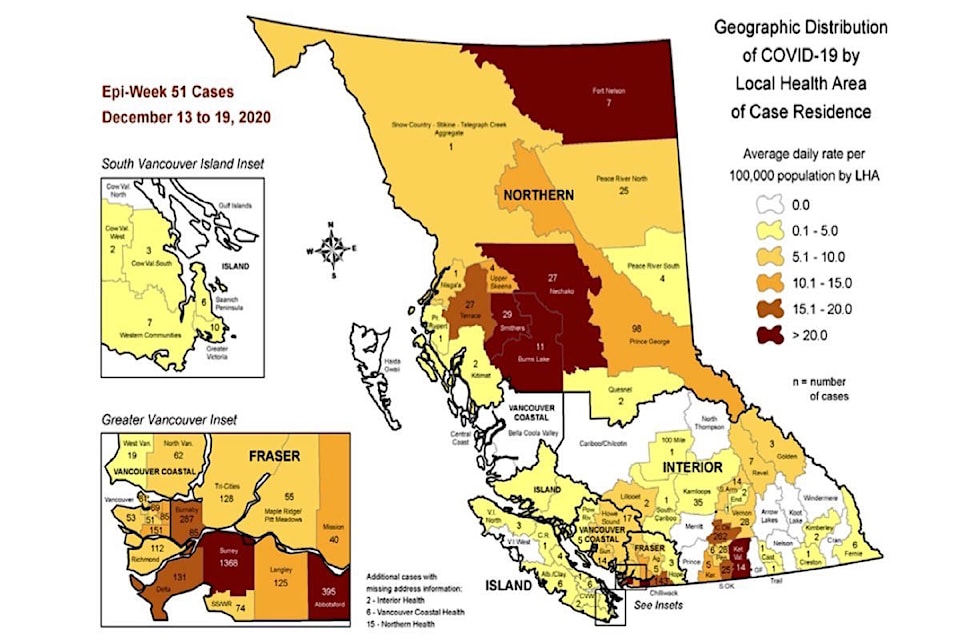
By the time B.C. public health officials started releasing more localized information on COVID-19 infections, people were familiar with hotspots like Surrey and Abbotsford in the Fraser Health region.
Add to that list Smithers, Burns Lake, Nechako, Fort Nelson in the north and in southern B.C., Kettle Valley. Those are the local health areas where average daily coronavirus case numbers are small, but among the highest as a share of population. And rural and remote locations mean greater difficulty in infection containment and contact tracing.
Presenting the latest epidemic modelling, provincial health officer Dr. Bonnie Henry cautioned that the localized case information is reported by where infected people live, and does not show where people picked up the SARS-Cov-2 virus while travelling.
“As the number of cases of COVID-19 have increased over the past number of weeks and months, we are now able to present data by local health area, and that is a more granular understanding of where cases have been,” Henry said Dec. 23. “I will remind people that this is our average daily rate per 100,000 population, and local health area represents the communities where people live who have tested positive for COVID-19. That is our convention across the country that we report by where people live.”
Most identified cases are from clusters or exposures to a known infected person, and industrial work sites and meat processing plants have been a particular issue in the second surge of the virus.
RELATED: Rapid-response paramedics sent to Fort St. James
VIDEO: First Nations elders urge caution in traditional language
Henry said the arrival starting next week of the more portable Moderna vaccine allows for targeted immunization in remote communities, where contact tracing has been most difficult.
“It comes in boxes of 1,200 doses, but we can break it down into as small as 100 doses and take that out to different parts of communities around the province,” Henry said. “So that means we can start to address some of the urgent needs that we have to protect people in some of our remote and isolated, particularly First Nations communities, and also residents of long-term care homes, where we know the virus is causing the most damage.”
The target for December to February vaccinations includes 25,000 people in remote and isolated Indigenous communities. They are not identified, but one of the first outbreaks that scrambled the province’s mobile response team was at Fort St. James in the Nechako health area.
@tomfletcherbc
tfletcher@blackpress.ca
Like us on Facebook and follow us on Twitter.