Aaron Craven was scared his elderly mother would not recognize him after months of being forced to communicate and connect through a third-floor window or Skype call at the beginning of the pandemic.
Since then, he has watched 83-year-old Patricia Craven, who has Alzheimers and lives at the Sunrise long-term care home in Vancouver, navigate through an unprecedented two years.
While able to today be at her bedside, Craven now wants policymakers to take responsibility for what he described as a horrific experience navigating visitation rules while trying to see his mother in long-term care.
Craven’s mother was diagnosed with Alzheimer’s at the same time her husband, Donald Craven, was diagnosed with dementia in 2016. Craven’s father died in 2018.
Craven remembers how his father would smile at him during the end-of-life palliative care stage. His mother’s conversation does not always make sense and she uses a wheelchair, but she knows when Craven is there to see her, he said.
“When she sees me, she still throws her arms around me to give me a hug, and gives me a nice big smile… Someone’s child is the last person they will ever forget.”
Craven recalled how months without in-person visitation affected his mother’s demeanor. He would walk by the care home to wave to the third-floor from the sidewalk, where care staff brought Patricia Craven to the window. With time, her expression became blank.
However, she lit up when she reunited with her son through a first-floor open window — she recognized Craven. Window visitation opened and closed in line with outbreaks – too often to count.
RELATED: B.C. retirement home residents fight province’s visitor restrictions
Essential visitor policy a challenge, says loved one
Craven first learned about essential visitor status when he called Vancouver Coastal Health to ask what he could do to see his mother during a no-visit period — he was desperate.
Craven was told he had to provide physical care, such as feeding or bathing, to apply for essential visits. Family visits were social visits. He was told they would try to make an exception for him, because essential visits were not for emotional needs.
“I had to go around the definition and say, ‘I am an essential visitor, I am her only child, I am her only family member. I can see the mental health toll this is taking on her, she knows something is wrong. I need to get in there and be a regular visitor as safely as possible.’”
Looking back, it felt like the red tape was a deterrent to families making a fuss about seeing their loved ones, he said.
The essential visitor category allowed a person paramount to a resident’s mental or physical well-being to provide for them while visitation was limited. Essential visit reasons can include physical care, supported decision-making, and communication or emotional support for people with disabilities, according to public health’s July 2021 visitation interpretive guide.
Craven feels future public health orders need to do a better job of balancing resident’s needs for family connection with outbreak safety.
Craven endorsed solutions like outdoor visits for masked and vaccinated family members if a facility did not want visitors to enter the building during an outbreak, but said the public health orders were not flexible enough to allow it.
RELATED: B.C. seniors worry more about death from loneliness than COVID-19
Survey highlights gaps, barriers
A survey released earlier this month by the Alzheimer Society of B.C. suggests many long-term care residents’ loved ones were told conflicting information about visitation rules.
Roughly half of people who responded to the survey said they were informed about the essential visitor policy, and those that were told about it were twice as likely to apply. Of the 86 people who applied and were denied essential visitor status, the most common reasons were that staff care was sufficient or the visit did not meet essential criteria.
Of the 499 British Columbians who completed the survey, roughly three-quarters were adult children, children in-law or spouses to a resident in long-term care. Roughly half of people said they applied for essential visitor status, and 65 per cent of those applications were successful, according to the Alzheimer Society report.

Alzheimer Society of B.C. CEO Jen Lyle said many people were told they had to do physical care for essential visits, but others received essential visitor status for emotional care without even applying. Some people were approved as essential visitors but were told they could not visit during an outbreak.
The 28 per cent of applications for essential visits listed physical care as a reason. The majority of people applied to help with a resident’s mental well-being. Lyle said applications that listed physical care were more likely to be successful. Spouses were more likely to be told about and successfully apply for visitor status than adult children.
Lyle said in-person visits with people with dementia are important, because they know who they are loved by even when their condition worsens. The public health orders took away resident’s autonomy, Lyle said. The family and resident would be involved in any other decision about care, but not the visitation public health orders.
“That comes back to respecting the fundamental rights that people living with dementia have, and they do not give up those rights when they’re moving into care,” she said.
Policies varied at different facilities, according to the survey. Some facilities allowed more than one essential visitor, so long as there was only one essential visit at a time. Other facilities only allowed one essential visitor, which forced residents to make impossible choices.
“We forced people to choose. Are you a mother first, or a wife first?” Lyle said.
Lyle said identifying essential visitors and designated visitors should be part of the admission process, and clearly communicated to the family. That way, the visitation plan is documented for any emergency. Craven does not know if he has essential visitor or single designated visitor status now, because it has not been a barrier to see his mother for so many months.
Craven does not want the full spectrum of opinions on COVID-19 to inform visitation rules, because he worries about others’ irresponsibility causing his mother to get sick. Some families harassed Sunrise staff about important rules like masking and gathering sizes.
“I just want the ministry to weigh the mental health aspect of its decisions… Our elected officials need to not write orders which only address physical needs. They need to look at the mental health aspect of family connection.”
Craven said his mother’s care home had trouble understanding how to apply the rules at times. The public health orders’ categories of visitors were not clear.
The most updated policy is outlined in a 21-page report from the ministry of health, published in March.
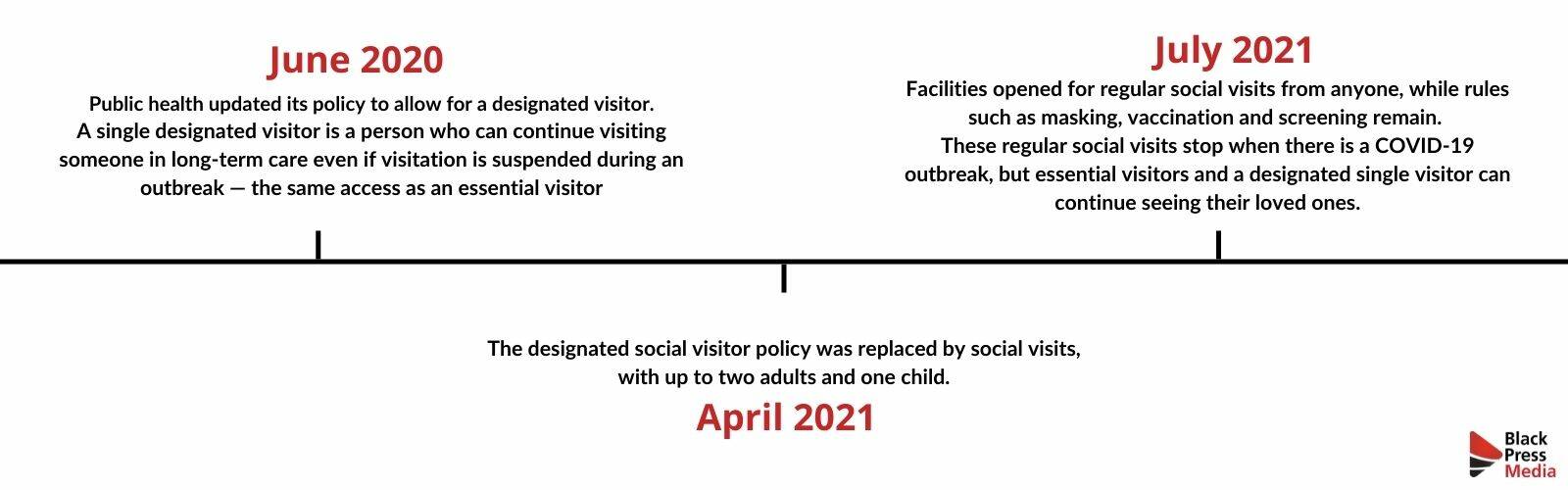
Visitation restrictions were updated or changed many times since March 2020. The first public health order only allowed essential visitors to see their loved ones in long-term care.
Black Press Media reached out to the health ministry for comment, but did not hear back by time of publication.
RELATED: Smiles abound as B.C. seniors in care get to see their families again
